A 49-Year-Old Woman with Chronic Abdominal Pain
September 7, 2022
A 49-year-old woman was referred to our tertiary care center for a second opinion on chronic pain symptoms in the abdomen, lower back, and left iliac fossa. On admission, she reported long-standing symptoms of constipation and recurrent urinary tract infection. These symptoms had developed after spondylodesis at the level of L5-S1 had been performed 3 years prior to address recurrent back pain after an earlier surgical procedure to treat herniated nucleus pulposus. Spondylodesis was performed with a combined anterior (i.e., left-sided retroperitoneal) and posterior approach and was complicated by retroperitoneal bleeding of unknown quantity. At 4 weeks after spinal surgery, the patient was readmitted to the hospital with left-sided hydroureteronephrosis. The abdominal computed tomographic (CT) scan at that time showed a left-sided parailiacal mass enveloping and constricting the left ureter (Fig. 1), for which a double-J stent was placed. The patient did not use methysergide or any other ergot derivative.
Based on the CT scan, the patient was diagnosed with retroperitoneal fibrosis.
After recurrent, left-sided hydronephrosis and multiple double-J stent placements, laparoscopic ureterolysis with omentoplasty was performed. However, hydroureteronephrosis recurred and abdominal pain persisted. The repeat abdominal CT scan showed a fibrotic strand adhering to the sigmoid. Explorative laparotomy was performed with mobilization of the sigmoid and rerelease of the left ureter. After this operation, there was no recurrence of hydronephrosis, but the patient still experienced pain symptoms. Laboratory investigation and abdominal CT scanning performed at our center on referral at 3 years after spinal surgery showed no abnormalities, in particular, no ureteral obstruction or retroperitoneal soft-tissue mass. Persistent pain symptoms and constipation were believed to be due to abdominal adhesions after multiple abdominal surgical procedures, and recurrent urinary tract infections were believed to be due to previous multiple stenting and repeated ureteral surgical procedures. Hence, no specific treatment was started. At the patient’s latest follow-up, she still had chronic pain symptoms but no recurrent hydroureteronephrosis.
Proceed to Discussion >>Reference: Buijs SM, Hendriksz TR, van Bommel EFH. Retroperitoneal fibrosis after spinal surgery: a report of 2 cases. JBJS Case Connect. 2021 Oct 27;11(4).e21.00269
This 49-year-old woman developed retroperitoneal fibrosis after spinal surgery. Our literature review identified 6 other patients who appear to have developed retroperitoneal fibrosis after spinal surgery. All had undergone an anterior lower interbody fusion, sometimes associated with posterior spine fusion. As anterior lower interbody fusion was the common denominator in these cases, it has been hypothesized that retroperitoneal instrumentation and manipulation caused chronic inflammation, fibroblast proliferation, and subsequent retroperitoneal fibrosis with external ureteral compression. Anterior lower interbody fusion is sometimes associated with substantial perioperative hidden blood loss, and retroperitoneal hematomas have been identified as a potential cause of retroperitoneal fibrosis. Other factors that might contribute to retroperitoneal fibrosis include low-grade infection, the use of metallic implants, the long duration of the surgical procedure, and the inclusion of L4-L5.
Of note, retroperitoneal hematoma may occur with posterior spine fusion if the vessels are torn during exposure of the lateral elements of the spine. Direct ureteral injury with spinal surgery with the posterior approach has also been described. Hence, we cannot exclude the possibility that the posterior approach was responsible for or contributed to retroperitoneal fibrosis development in our patient. However, this seems less likely because anterior lower interbody fusion was the common denominator in all reported cases, and none of the patients underwent posterior spine fusion as the only procedure. In 6 reported cases, the diagnosis of retroperitoneal fibrosis was suspected on the basis of the results of intravenous pyelogram studies, in which an obstruction with stenosis and/or medial deviation of the ureter(s) with overlapping of the spine was recognized as a classic sign of retroperitoneal fibrosis. Diagnosis was subsequently confirmed by exploratory laparotomy and surgical biopsies. In 2 more recent cases, retroperitoneal fibrosis diagnosis was based on the results from the abdominal CT scans that showed a typical well-delineated retroperitoneal soft-tissue mass.
Nowadays, after careful exclusion of any sign of malignancy, characteristic findings with the contrast-enhanced abdominal CT scan will usually suffice to establish the diagnosis of retroperitoneal fibrosis. Histological confirmation is usually needed only in cases with atypical radiological findings. In the case of severe renal failure precluding the use of intravenous contrast, magnetic resonance imaging may also provide a characteristic picture. Presentation signs in the reported cases were typically recurrent urinary tract infections and pain, varying from the flank, abdomen, and back, sometimes accompanied by constipation. Most patients sustained hydroureteronephrosis, which disappeared after ureterolysis and/or retroperitoneal fibrosis-specific medical treatment. Medical treatment with initial high-dose prednisolone or with fixed-dose tamoxifen, if needed with (urgent) renal drainage, is nowadays the treatment of choice for retroperitoneal fibrosis because it suppresses the chronic inflammatory reaction and thereby typically leads to the amelioration of signs and symptoms and to the regression of the retroperitoneal soft-tissue mass. Mass regression is often such that ureteric obstruction resolves, thereby precluding the need for urologic surgery. During follow-up, no recurrence of hydroureteronephrosis and/or pain symptoms were reported in 7 of the 8 reported cases after retroperitoneal fibrosis-specific surgical or medical treatment. However, 1 patient who underwent multiple operations sustained persistent chronic pain, and 1 other patient sustained irreversible kidney damage.
In conclusion, retroperitoneal fibrosis may be a long-term complication of anterior lower interbody fusion, a procedure that may involve retroperitoneal manipulation and instrumentation, and may be accompanied with retroperitoneal blood loss, all of which may lead to chronic inflammation, fibroblast proliferation, and subsequent retroperitoneal fibrosis. Strategies to mitigate this reaction include limiting operative time, scrupulous adherence to aseptic technique, and interventions to limit intraoperative blood loss. In addition, a low threshold for performing abdominal CT scanning is warranted for the early recognition and treatment of retroperitoneal fibrosis.
Reference: Buijs SM, Hendriksz TR, van Bommel EFH. Retroperitoneal fibrosis after spinal surgery: a report of 2 cases. JBJS Case Connect. 2021 Oct 27;11(4).e21.00269
What is the diagnosis?
Iliac pseudoaneurysm
Ureteral neoplasm, suggestive of leiomyoma
Transitional cell carcinoma of ureteral origin
Retroperitoneal fibrosis
Chondrosarcoma arising in a pelvic osteochondroma


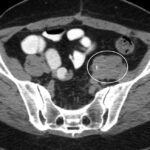 Fig. 1
Fig. 1