An Eighty-three-Year-Old Man with Pain and Immobility Following Total Knee Arthroplasty
October 15, 2014
An eighty-three-year-old man with multiple medical comorbidities, including atrial fibrillation, underwent a primary right total knee arthroplasty. A tourniquet was used only during the cementing portion. No drain was used. There were no perioperative complications. Preoperatively, the patient had been on chronic warfarin therapy for the atrial fibrillation, but the warfarin had been stopped for six days before the procedure. In the five months prior to stopping the warfarin, the international normalized ratio (INR) ranged from 1.7 to 2.1. After surgery, the patient was treated with enoxaparin while hospitalized, and warfarin therapy was resumed. On postoperative day three, the skin around the incision appeared slightly swollen and ecchymotic but was within normal expectations, and the patient was discharged home. On postoperative day four, the patient presented to the emergency room because of increased pain and inability to mobilize, and he was admitted to the hospital. The knee was swollen and mildly erythematous and had some new hemorrhagic blisters. On postoperative day five, blisters were noted on the anteromedial side of the knee. After more blisters were evident the following day, they were drained at the bedside. On postoperative day seven, new blisters were noted posteriorly, and the skin beneath the old blisters appeared darker. On postoperative day eight, the INR peaked at 2.4 and the warfarin was discontinued. The INR steadily declined to normal values over the next five days. The patient was given fresh-frozen plasma and began enoxaparin therapy. Figure 1 shows the appearance of the knee at this time. The blisters kept enlarging for two more days before they appeared to stabilize on postoperative day eleven. The skin and soft tissues, however, continued to deteriorate until there was circumferential full-thickness necrosis around the knee (Fig. 2).
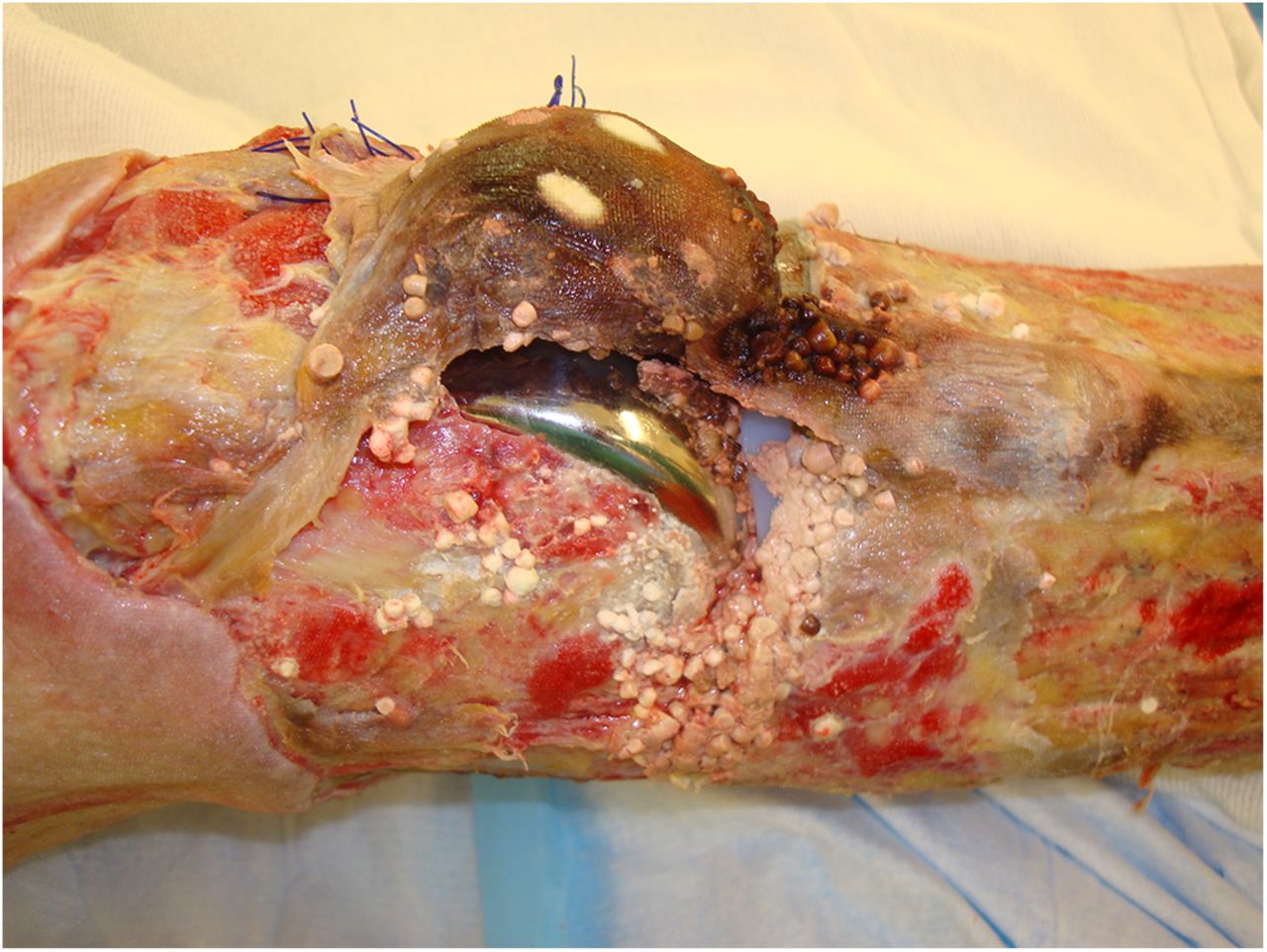
Several specialists were consulted, including hematologists and oncologists, and a full workup was initiated. D-dimer and fibrinogen levels were both elevated. The hemoglobin remained stable and the platelet count was normal to elevated during the hospitalization. Knee joint fluid, blood, and urine cultures were negative for infection. Cryoglobulin, antinuclear antibody, neutrophil cytoplasmic antibody, and lupus anticoagulant studies were negative. Ultrasound studies were negative for deep vein thrombosis or arterial stenosis. The skin and soft-tissue necrosis stabilized, and the patient was discharged on postoperative day twenty-two. Plans were made to take him to the operating room for surgical debridement at a later date. Excisional debridement of the wound and eschars was performed on postoperative days forty-one and forty-three. At the first debridement, the necrosis was noted to be circumferential, starting from just above the patella to 7 cm distal to the patella. A small area of skin in the popliteal region appeared viable. Debridement was carried down to the fascia. At the second debridement, the area of necrosis was estimated to be 40 cm in length and 25 cm circumferentially, with involvement of the joint capsule. On postoperative day forty-five, the patient was transferred to a tertiary center. Protein C, protein S, antithrombin III, and factor-V Leiden studies were all normal. The patient was taken to the operating room on postoperative day forty-eight; both orthopaedic and plastic surgeons were present for the irrigation and debridement. The skin and soft-tissue necrosis was extensive, and flap coverage with use of the gastrocnemius was deemed nonviable. The extensor mechanism (the patellar tendon, the patella, and the quadriceps tendon) was necrotic as well. Additional treatment options were discussed with the patient after the surgery, and he elected to proceed with a transfemoral amputation. This occurred on postoperative day fifty-two (Fig. 3). The patient was stabilized and discharged home on postoperative day fifty-five.
Proceed to Discussion >>Reference: Wang J, Giordani M, Pereira G. Warfarin-induced skin necrosis after total knee arthroplasty: a case report. JBJS Case Connect. 2014 Jul 23;4(3):e60.
Coumarin-derivative-induced skin necrosis involving the breast was reported as early as 1943. Today, warfarin is the most common coumarin derivative used for prophylaxis and treatment of thromboembolic disease. Multiple national guidelines have deemed it an acceptable agent for chemical prophylaxis of deep vein thrombosis and pulmonary embolism after orthopaedic surgery. Since 1943, more than 200 cases of warfarin-induced skin necrosis have been reported, and many aspects of the disease have been identified. The estimated percentage of patients taking warfarin or another coumarin derivative who will experience this complication is 0.01% to 0.1%. Women develop this complication more often than men; common characteristics of those who are affected most often include women who are middle-aged and obese, as well as those undergoing treatment for pulmonary embolism or thrombophlebitis. The most commonly affected areas are regions with substantial adipose tissue (e.g., the breast, buttocks, hips, and thighs), although other areas have been reported as well. Deficiencies in protein C, protein S, and antithrombin III are associated, but not always present, with the complication. The pathophysiology, while not completely understood, is thought to be an imbalance in the procoagulant-anticoagulant system due to a relative reduction in protein C compared with the other vitamin K-dependent coagulation factors, leading to a transient state of hypercoagulability and thrombus formation. Dermatologic lesions usually appear within ten days of initiation of warfarin, although much longer time periods have also been reported. The initial lesions are painful and often erythematous, followed by the development of hemorrhagic blisters and bullae and/or petechiae, which eventually progress to necrotic eschars. The differential diagnosis is broad, including but not limited to subcutaneous hemorrhage, calciphylaxis, arterial occlusion, purple toe syndrome, purpura fulminans, necrotizing fasciitis, cryoglobulinemia, cholesterol microemboli, disseminated intravascular coagulation, and heparin-induced thrombocytopenia and thrombosis syndrome. Histologically, the lesions appear as an aseptic noninflammatory thrombotic vasculopathy with focal epidermal necrosis, with fibrin thrombi that occlude dermal and subdermal venules. When recognized, warfarin-induced skin necrosis is treated with a combination of warfarin cessation, administration of vitamin K or fresh-frozen plasma to reverse the effects of warfarin, administration of protein C and/or protein S if the patient is deficient, administration of heparin or another anticoagulant since the primary pathophysiology is thrombosis formation, and local wound care. Surgical treatment is required in over 50% of patients, and includes debridement, soft-tissue coverage, and sometimes mastectomy or amputation. If progressive and uncontrolled, the lesions can lead to sepsis and even death. The patient described in our case report does not fit very many of the common characteristics that have been previously reported. He was a nonobese elderly man undergoing prophylactic treatment for atrial fibrillation and had recently had total knee replacement surgery. He had stopped taking warfarin before the surgery, but it was resumed later, which is consistent with reports of warfarin-induced skin necrosis developing in patients after a brief hiatus from warfarin or after subsequent initiation of warfarin therapy. In contrast with the other two case reports previously published in the orthopaedic literature, the necrosis was localized to the surgical region only, although another study documented that necrosis manifests as a single lesion in over 50% of reported cases. Warfarin-induced skin necrosis is essentially a diagnosis of exclusion. It remains unclear as to exactly why it developed in our patient. As hypothesized in previous studies, one possible explanation is that the abrupt cessation and reinitiation of warfarin led to a hypercoagulable state and subsequent formation of thrombi, with the macroscopic changes declaring themselves days later. This may have been exacerbated by the use of perioperative antibiotics and the patient’s poor nutritional status (as evidenced by low prealbumin and albumin levels), both of which can lead to a decrease in vitamin K and possibly a relatively greater decrease in vitamin-K-dependent anticoagulants (proteins C and S). Given how common total joint arthroplasties are, as well as how commonly warfarin is used for chemical thromboembolic prophylaxis, it is imperative for orthopaedic surgeons to be aware of warfarin-induced skin necrosis as a potential adverse reaction and complication, and to understand how to approach it, especially since there is no effective screening method. Caution should be used in patients with known deficiencies in protein C, protein S, antithrombin III, and vitamin K by using a lower initial loading dose and bridging with enoxaparin, or with use of an alternative agent altogether. While there may be a paucity of evidence that the various therapeutic approaches affect eventual outcome after irreversible signs of skin injury are present, the vast majority of the literature advocates early clinical suspicion and prompt diagnosis as imperative for optimizing patient outcome. The three earliest clinical manifestations of warfarin-induced skin necrosis are pain, erythema, and the development of blisters. Although pain and erythema are relatively common after total knee arthroplasty in patients who do not develop this complication, these symptoms should be taken seriously and closely monitored, especially when out of the ordinary, since the complication can be prevented if treated early.
Reference: Wang J, Giordani M, Pereira G. Warfarin-induced skin necrosis after total knee arthroplasty: a case report. JBJS Case Connect. 2014 Jul 23;4(3):e60.
Clostridial infection
Popliteal artery thrombosis
Ischemic skin necrosis
Warfarin-induced skin necrosis
Factor-V Leiden-related compartmental syndrome

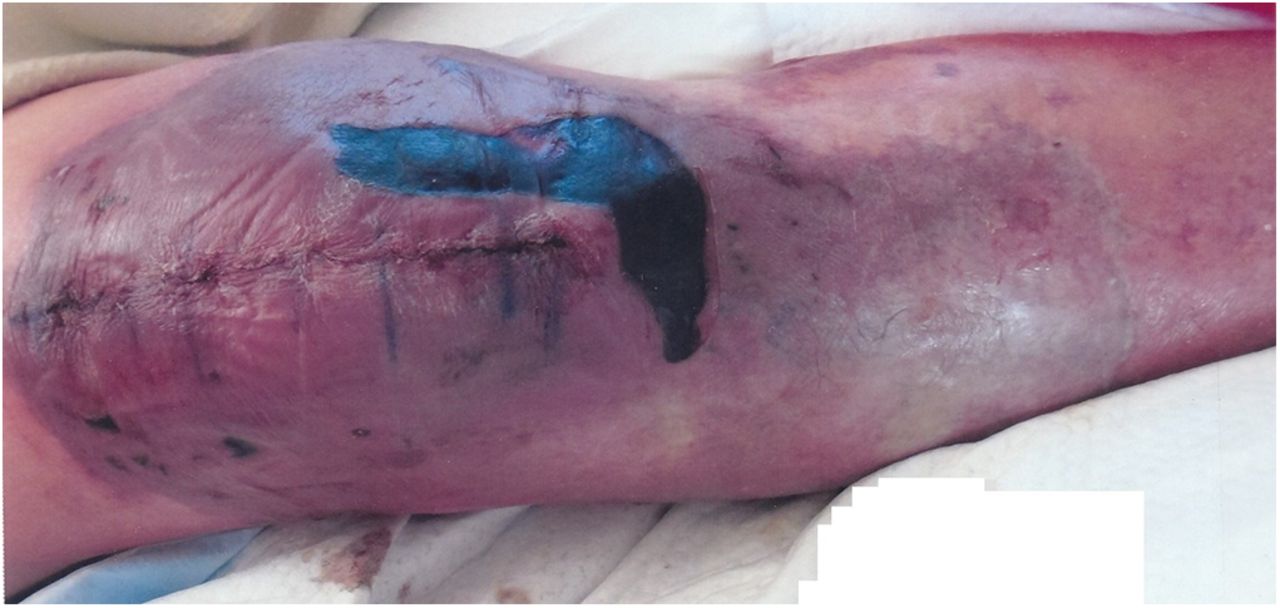

 Fig. 1
Fig. 1 Fig. 2
Fig. 2 Fig. 3
Fig. 3